Development and Testing of CAR-NK Cells for Relapsed Pediatric AML
Shannon Reinert, MD; Mark Wunderlich, MS; Benjamin Mizukawa, MD
CAR-NK Cell therapy could be an alternative to CAR-T Cells for relapsed pediatric AML. Further work is needed to efficiency generate CX3CR1 targeting CAR-NK cells.
Shannon Reinert, MD
Abstract
Background: Chimeric Antigen Receptor T (CAR-T) cells are engineered T cells that have been extremely effective in treating relapsed or refractory hematologic malignancies in recent years. However, treatment can have a number of serious side effects. Recently, focus has shifted from CAR-T cells to CAR-NK cells. By studying the genes of patients with relapsed AML at CCHMC, we have previously discovered certain genes that are significantly overexpressed in AML cells. These genes were further filtered based on favorable tissue expression patterns (highest in the blood, lower in other tissues), resulting in identification of potential targets for CAR-NK development. CX3CR1 is a chemokine receptor with published cancer and AML associations.
Objective: We aimed to generate CAR-NK cells to target CX3CR1, along with a CD33-targeting CAR-NK cell line to serve as a positive control. Prior to testing in vivo efficacy in PDX models, we planned on using an in vitro cytotoxicity assay to demonstrate efficacy.
Methods: Lentiviral transduction was employed to create CAR-NK cells. Experiments were conducted with two unique NK cell lines and a number of different CAR-containing lentiviral vectors. Flow cytometry was used to determine transduction efficiency. Prior to effective CAR-NK cell generation, a proof-of-concept experiment was conducted to test our in vitro cytotoxicity assay. Target cells (one of two different AML cell lines) were combined with effector cells (either NK-92 or KHYG-1 NK cells) at different effector:target ratios. Medium alone was added to target cells for control. Flow cytometry and annexin V were used to identify apoptosis.
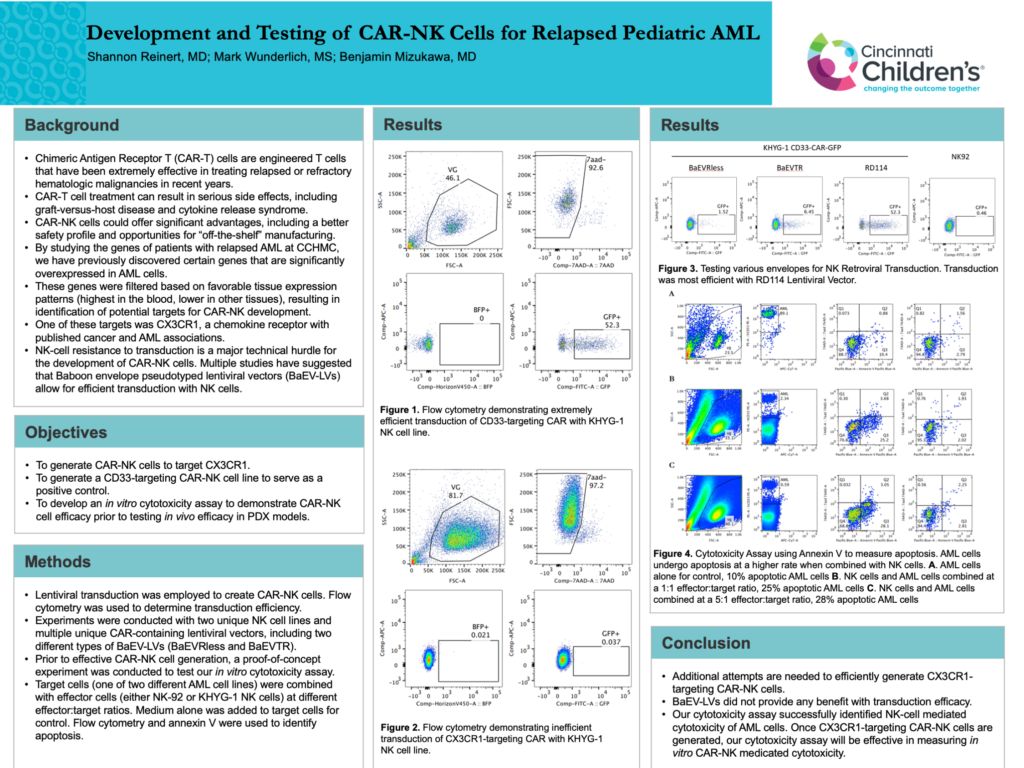
Results: Using flow cytometry, we demonstrated extremely efficient transduction of CD33-targeting CAR with NK cells, to severe as a positive control. Using a number of different NK-cell line and lentivirus vector combinations, we did not yet demonstrate efficient transduction of CX3CR1-targeting CAR with NK cells. Using our cytotoxicity assay, we demonstrated that AML cells underwent apoptosis at higher rates when combined at a higher effector:target ratio.
Conclusions: Additional attempts are needed to efficiently generate CX3CR1-targeting CAR-NK cells. Our cytotoxicity assay successfully identified NK-cell mediated cytotoxicity of AML cells. Once CX3CR1-targeting CAR-NK cells are generated, our cytotoxicity assay will be effective in measuring in vitro CAR-NK medicated cytotoxicity.